Following cataract surgery, the vitreous loss is linked to a poor visual outcome. Experienced surgeons and those who perform a large number of cataract procedures are less likely to encounter vitreous loss. Less experienced surgeons may use risk categorization tools to help them avoid high-risk patients. Prior to cataract surgery, patients must be counseled about the potential dangers and complications of vitreous loss.
It is vital for the surgeon to avoid practices that increase the risk of an eye catastrophe when a vitreous loss occurs. Non-vitrectomy procedures to remove lens components from the posterior area include phacoemulsification in the presence of vitreous.
There are benefits to doing an anterior vitrectomy via the pars plana channel rather than the anterior chamber, and sutureless 23-gauge instruments may help with this. Retinal detachment, subsequent glaucoma, and cystoid macular edema are all linked to lens nuclear fragment displacement into the vitreous. It is recommended that these eyes be treated by a retinal surgeon as soon as possible.
The vitreous body is protected by the posterior lens capsule, which is an anatomical barrier that prevents lens fragmentation, aspiration, and intraocular lens implantation stressors. Capsule rupture and vitreous loss occurred in 4.4 percent of participants in the UK national cataract surgery study from 1997 to 1998.
Other studies have shown rates ranging from 8.22 to 0.45 percent of participants. Vision-threatening complications such as cystoid macular edema, retinal detachment, and endophthalmitis are all linked to vitreous degeneration. (2), (3), (4), (5), (6), (7) When the posterior capsule is disrupted, lens components may be displaced into the posterior segment, resulting in an even worse prognosis for those eyes.
Prevention
The finer points of safe cataract surgery are discussed in the current literature and are beyond the scope of this article.

The surgeon’s experience,6 surgical volumes (number of cataract surgeries done per surgeon each year),12, 13, and the complexity of cases or case-mix all influence vitreous loss. Prior to cataract surgery, scoring methods offer a quantified estimation of risk in specific cases. Such risk classification allows for the prediction and avoidance of complications by adequate patient preparation, anesthetic type, and surgeon selection.
Even experienced consultants had an 8% vitreous loss rate and a 4% fallen lens nucleus rate in high-risk eyes, according to Muhtaseb. Surgeons competent in vitrectomy and the removal of misplaced lens components from the posterior area seem to be the best candidates for cataract surgery in such eyes.
While the importance of the capsulorhexis in the success of cataract surgery has been rightly emphasized17, the quality of the capsulorhexis may be determined considerably earlier in the procedure by variables such as patient preparation, and anesthetic selection, and wound architecture. In high-risk eyes, such as after vitrectomy18, problems may occur even with perfect capsulorhexis, when an unstable anterior chamber depth causes anterior chamber depth changes, pupil constriction, and patient discomfort. 19 It’s critical to comprehend how to handle these eyes.
Management of the patient
Cataract surgery is not a common operation, although it has become commonplace. Managing a significant intraoperative complication will be simpler for the patient if informed consent includes a discussion of predicted vitreous loss, lens matter displacement, and failure to implant an intraocular lens. This will reduce patient anxiety and aid in the development of trust between the patient and the physician during and after the cataract surgery process. Patients want to know about unusual outcomes; 93.5 percent want to know if the risk is one in 50, and 62.4 percent want to know if the risk is one in 1000. However, recall accuracy of consent information is poor, especially for serious issues, posing a challenge in preparing patients for potentially dangerous procedures. You can also read about Nucific BIO X4 Probiotic Review – Does It Really Work by clicking here.
Management: keeping a close check on things
A minor but rapid alteration in the internal conditions of the eye will signal the presence of vitreous loss. Sudden chamber deepening altered lens nucleus mobility, excessive sideways displacement of the nucleus, the sudden appearance of a red reflex, and abnormal movement of structures (for example, the pupil margin) remote from instruments in the anterior chamber caused by traction transmitted through vitreous strands are some of the signs that may be seen.
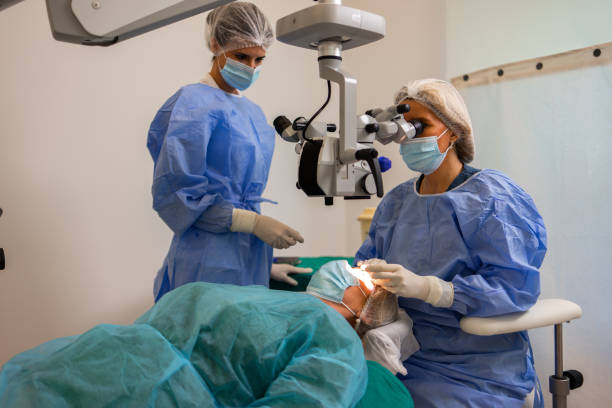
If phacoemulsification is still being done, it should be stopped and the probe is gently withdrawn from the eye in a way that does not put any strain on the vitreous. When the phacoemulsification probe is withdrawn, a viscoelastic substance may be injected into the anterior chamber to help prevent vitreous prolapse and stabilize any leftover lens components. It is vital that the surgeon then meditates for a few moments. Setting up the vitrectomy device and, if required, administering a sub-anesthetic may be done while the condition is being examined. The lens nucleus or significant parts of lens material may sink posteriorly due to a delayed reaction at this point. This is a controllable problem with a generally positive result. Precipitate and strong efforts to retrieve lens fragments through an anterior method are harmful.
Vitreous loss treatment aims to remove any vitreous from the anterior chamber and surgical site so that cataract surgery may be completed and an intraocular lens can be implanted safely. Depending on the surgeon’s competence and the complexity of the case, any, all, or none of these activities may be performed by the main surgeon. A vitreous cutter and a separate infusion delivered by an anterior chamber maintainer should be used to remove the vitreous. It is not recommended to employ a coaxial infusion sleeve around a vitreous cutter because it causes a flow conflict between infusion and aspiration, and control of intraocular pressure is lost each time the cutter is removed from the eye.
A shortcoming of so-called “dry” vitrectomy operations is their inability to maintain a stable intraocular pressure. The cutter should be placed via the pars plana to collect vitreous from the anterior chamber, utilizing either an anterior chamber or pars plana infusion. 25 This reduces anterior chamber manipulation, vitreous incarceration in the corneal incision, and the ability to remove vitreous deep beyond the posterior capsule, which is more difficult and dangerous when the cutter is entered via the anterior chamber. Triamcinolone particles may be used to view vitreous strands in the anterior chamber, although they aren’t necessary.
A 25-gauge needle was used for sutureless vitrectomy. The bigger 23-gauge sutureless devices provide greater control and may be more successful in dealing with vitreous and retained lens material. For removing soft lens debris, the vitrector is an ideal instrument. Nuclear debris may be emulsified and aspirated by reintroducing the phacoemulsification probe after the anterior chamber has been completely cleansed of vitreous, or intact nuclear fragments can be removed via an extended incision. Viscoelastic or a lens glide29 may be employed to stabilize nuclear pieces before removing them from the anterior chamber.
Forceful efforts to retrieve nuclear fragments that are moved posteriorly past the plane of the posterior capsule without pars plana vitrectomy may result in extensive retinal tears and detachment.


